Pregnancy Medical Home: Improving Maternal & Infant Outcomes in the Medicaid Population

June 2021 PMH Data Brief
Click to download CCNC's latest data brief:
"The Maternal-Infant Impactability Score™ (MIIS) for Care Managers: A Demonstrated Approach for Reducing Low Birth Weight Through Pregnancy Care Management"
MIIS Implementation
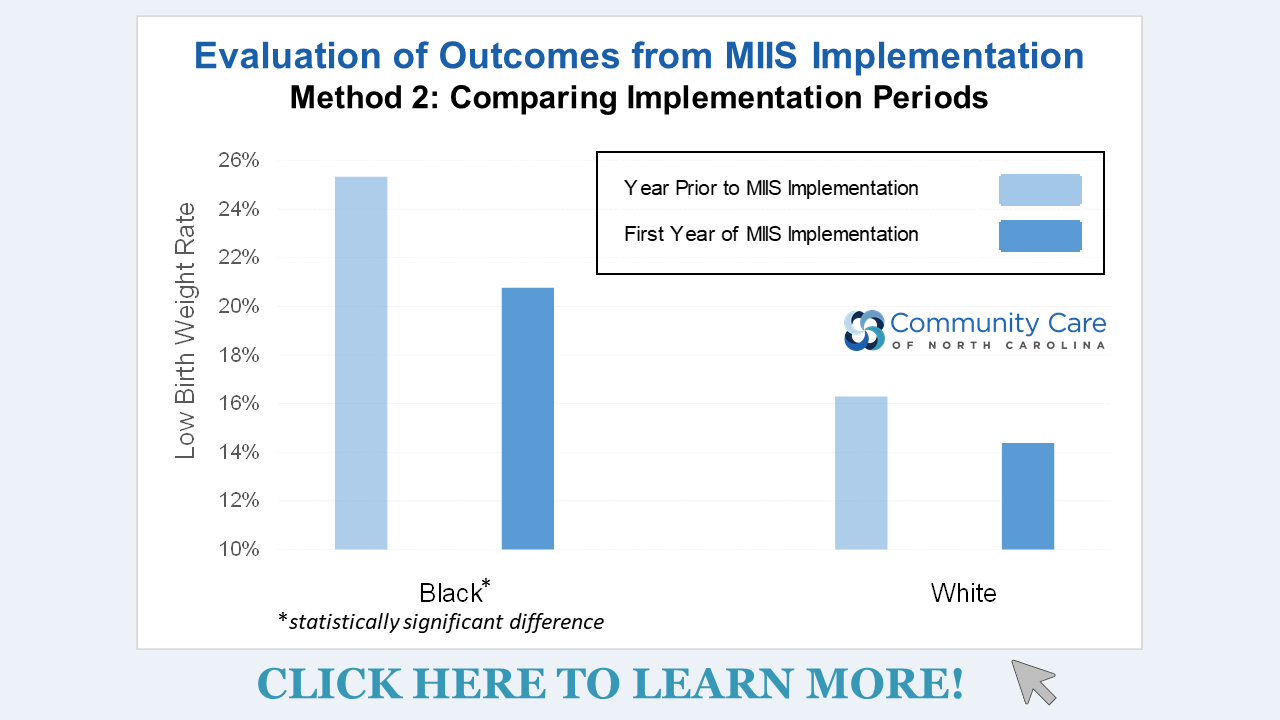
Community Care of North Carolina (CCNC) launched the Pregnancy Medical Home (PMH) program in 2011, to enhance access to comprehensive care for pregnant Medicaid beneficiaries and to improve birth outcomes. The PMH program promotes evidence-based, high-quality maternity care in more than 400 practices across the state. PMH practices represent 95% percent of prenatal care providers who serve the Medicaid population.
NASEM presentation by Dr. Kate Menard
CCNC gives presentation on advancing maternal health equity and reducing maternal mortality during a workshop hosted by the National Academies of Sciences, Engineering & Medicine (NASEM). The PDF presentation by M. Kathryn Menard, MD, MPH, distinguished professor of maternal-fetal medicine at UNC Chapel Hill and medical director of CCNC's Pregnancy Medical Home program, can be found alongside additional information on NASEM's website here.
